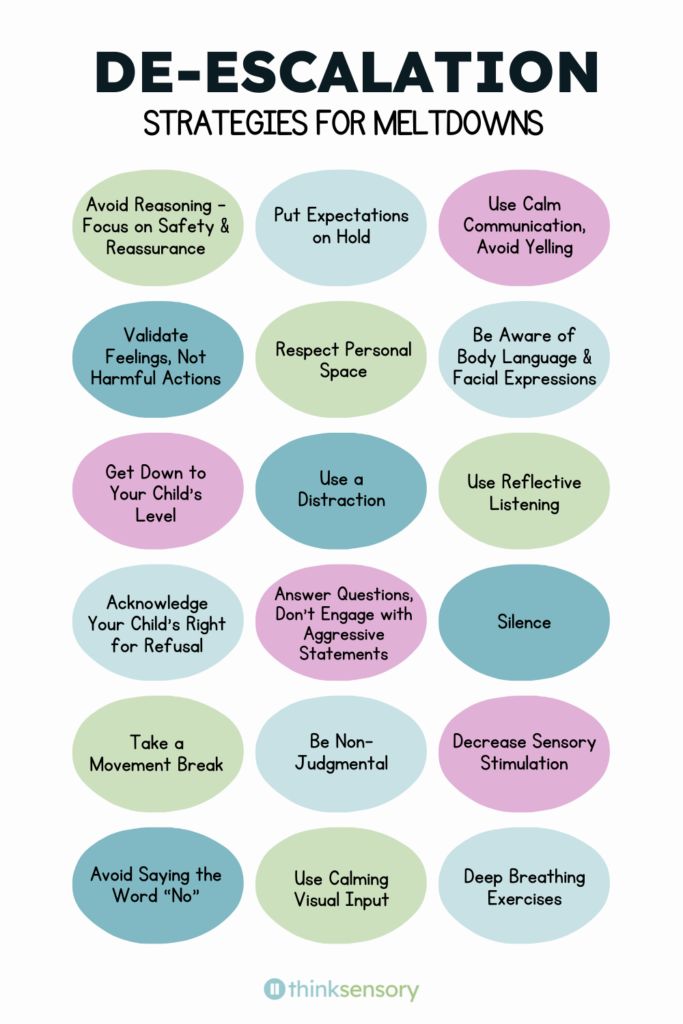
18 Effective De-Escalation Strategies For Defusing Meltdowns
What’s inside this article: An overview of the escalation cycle, how the nervous system responds during stress and what that means for your child’s behavior, and evidence-based, supportive de-escalation strategies to help you compassionately support your child during meltdowns and outbursts.
Understanding Meltdowns
As a parent, it’s important to know some safe, helpful de-escalation strategies for meltdowns.
Sometimes, when children become extremely overwhelmed or they’re experiencing sensory overload, they have a meltdown where they become so dysregulated that their bodies react automatically.
This is an automatic nervous system response and not something our kids can consciously control.
These situations are stressful and overwhelming for everyone involved and could potentially lead to safety risks for both your child and bystanders.
Knowing some de-escalation strategies will help you provide a supportive response to your child during these challenging moments.
The Escalation Cycle
Although meltdowns may seem unpredictable or like they happen out of nowhere, there is a clear pattern that happens before, after, and during a meltdown.
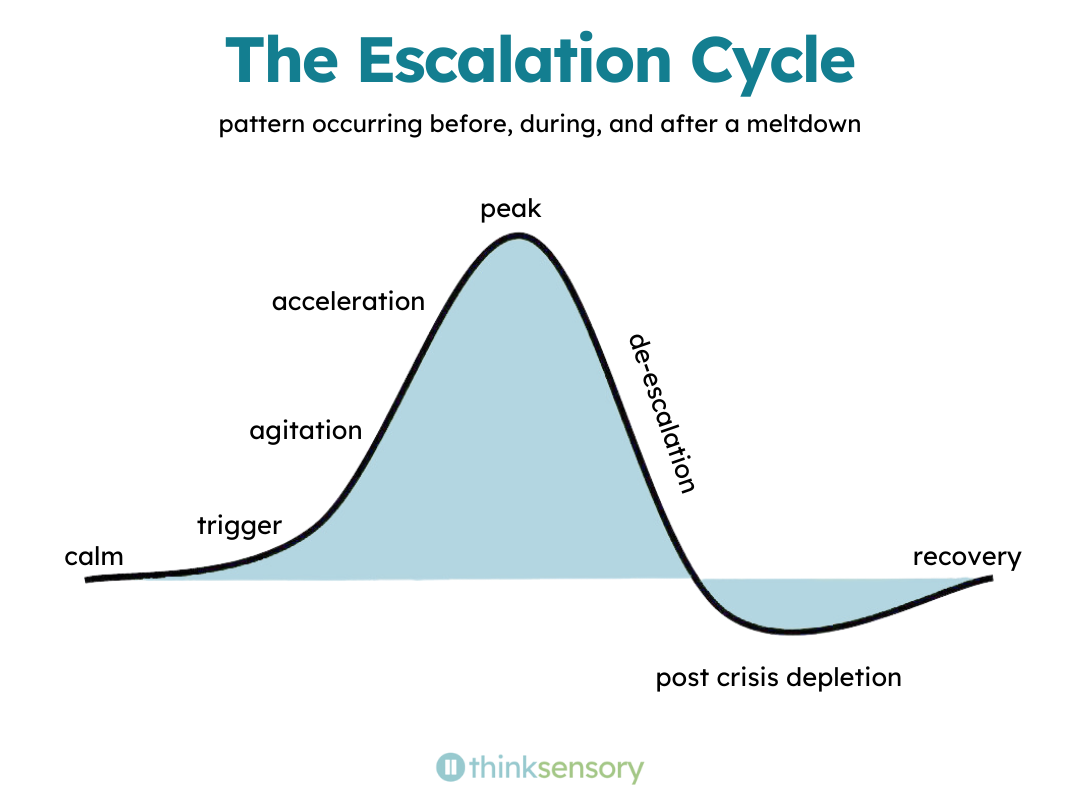
The escalation cycle is something I talk about in a lot of my posts, and familiarizing yourself with each of the stages and the different strategies for each stage will help you not only respond to meltdowns but also learn to support your child proactively, reducing their frequency.
Equally important to being able to identify each stage of the escalation cycle is knowing which non-violent crisis intervention strategies work for each stage.
There are approaches from crisis intervention frameworks that help keep everyone safe during meltdowns, and you should be using them alongside your de-escalation strategies. If you’re interested in learning more about safe, non-restrictive crisis support, the Alliance Against Seclusion and Restraint is a great resource.
Take a few minutes to read this list of 6 crisis support strategies to use during meltdowns.
Parents and caregivers can use these strategies to help keep their child(ren) safe during highly stressful or challenging moments.
What Happens in the Nervous System During a Meltdown
You might have seen the popular “three brain” diagrams floating around the internet that divide the brain into a thinking part, a feeling part, and a survival part.
While that model was useful for a long time, neuroscience has moved past it. The brain doesn’t actually work in neat layers that shut each other off, so doing so is a bit of an oversimplification of what’s really going on.
But here’s what IS happening, and why it matters for how you respond to your child.
Everyone’s nervous system has a built-in alarm system. When the brain detects a threat (whether that threat is real or just perceived), it activates the sympathetic nervous system, which is the system responsible for your fight, flight, and freeze responses.
This instantaneously FLOODS the body with stress hormones like adrenaline and cortisol.
When this happens, several things change all at once.
- Heart rate increases
- Breathing gets faster
- Muscles tense up
- The prefrontal cortex – the part of the brain responsible for executive functions like planning, decision-making, problem-solving, impulse control, logic, reasoning, and communication – becomes significantly harder to access.
It doesn’t shut off completely, but its capacity is drastically reduced. Just how reduced depends on a lot of factors – the individual person, how dysregulated they are, what triggered the response, and how much capacity they had going into the situation.

Think about your own experience for a second. If someone startled you unexpectedly, your heart might race for a minute or two and then you’d recover pretty quickly. But if something truly caught you off guard – a horrible moment that made your knees buckle, your vision go fuzzy, your whole body react before you could think – that takes much longer to come back from.
You’ve probably experienced both ends of that spectrum as an adult with a fully developed brain and years of life experience to pull from.
Now think about that from a child’s perspective. Their prefrontal cortex is still developing. They have fewer experiences to reference, fewer coping strategies to draw from, and less capacity to process what’s happening to them. Something an adult might see as “minor” – the wrong color cup, a change in routine, a seam in a sock – could genuinely be one of the most distressing things that child has experienced. They don’t have the context yet to rank it as small.
And here’s the part that’s hard to sit with but important to understand: physiologically, what’s happening in your child’s body during a meltdown over that “wrong cup” feels the same as what happens in your body during your worst moments.
The racing heart, the overwhelm, the inability to think clearly – that’s the same nervous system response. It doesn’t scale to how “valid” the trigger looks from the outside. The body doesn’t care whether the threat is “real enough” by adult standards. It just responds.
This is why your child can’t think clearly, communicate effectively, or respond to logic during a meltdown. It’s not a choice. Their nervous system has shifted into a protective state, and their brain is prioritizing survival over everything else.
Here’s another analogy that can help with understanding how the nervous system can react severely to something “minor”. Think of it like having an alarm system on your home to protect you from burglars, but it’s programmed to be so sensitive that it goes off any time a bird lands on your patio. The alarm is doing its job – it’s just responding to something that doesn’t actually require that level of response.
For many kids, especially neurodivergent kids, this alarm system can naturally be more sensitive. Sensory input, unexpected changes, demands, social overwhelm, or internal experiences like hunger or fatigue can all trigger the nervous system to respond as if there’s a real threat when there’s really just a bird on the patio. But the feelings they experience in their body are the same for both scenarios.
(I have some free resources for helping kids – and parents – better understand fight or flight here. )
What This Looks Like in Kids
When the nervous system is activated, you’ll see different protective responses depending on the child.
Fight responses might look like hitting, kicking, biting, screaming, throwing things, or pushing. From the outside, these can be perceived as aggression or defiance, but they’re actually the nervous system’s way of trying to protect the child from a perceived threat.
Flight responses might look like running away, hiding, trying to escape the situation, or becoming very physically restless.
Freeze responses might look like your child going completely still, becoming non-responsive, being unable to speak or move, or appearing to zone out or “shut down.” This one is important to recognize because a lot of parents and caregivers aren’t aware that freezing is a stress response too. If your child goes quiet and still during an overwhelming situation, that’s their nervous system at work, just like the child who screams and kicks. They need the same level of support.
During any of these states, your child has significantly reduced access to the skills they normally use – reasoning, communication, emotional regulation, following directions.
They may seem like they’re being uncooperative, demanding, or “difficult,” but what’s actually happening is that their nervous system has taken over and they’re doing the best they can with the resources available to them in that moment.
This is why, during a meltdown, it’s important to remain calm and focus on safety until the stress response has passed.
You absolutely can and should set boundaries, communicate clearly, tell your child “no,” if you need to, and guide them. You just need to wait until their nervous system has calmed enough for the prefrontal cortex to come back fully online. Otherwise, those conversations not only won’t land. They could escalate the situation.
Co-Regulation: Why Your Calm Matters
You’ll notice throughout this article that a lot of the strategies come back to one thing: staying calm yourself. There’s a reason for that.
Kids learn to regulate their emotions through co-regulation, which is the process of using the calm, regulated presence of another person to help settle their own nervous system.
This is how emotional regulation develops in the first place. Babies and young children can’t regulate on their own at all – they rely entirely on their caregivers to help bring them back to a calm state.
As kids grow, they gradually build the ability to self-regulate, but co-regulation doesn’t stop being important just because a child gets older. The need for co-regulation support extends well beyond early childhood, and that’s completely normal. Even adults rely on close friends, family and partners during emotional moments.
If you were having a really bad day and you went to your spouse or your best friend for comfort (co-regulation!) and they reacted by getting upset or angry with you, that would make the situation worse and make you feel much worse, too.
So when you stay calm during your child’s meltdown, you’re not just “keeping it together.” You’re actively providing the external regulation your child’s nervous system needs in order to begin calming down. Your steady presence is one of the most powerful de-escalation tools you have.
Understanding the “Point of No Return”
When your child reaches the point of a full meltdown, it’s important to recognize that there is no magic solution or quick fix to stop it instantly.
I know—as a parent, that’s not what you want to hear. It’s incredibly tough to watch your child struggle and not be able to immediately “fix” things. And it is also incredibly tough to keep regulated as you ride that wave with them.
But, at this stage, the best approach is simply to safely get through it together.
The de-escalation strategies outlined here are not about ending a meltdown instantly but about supporting your child compassionately through these difficult moments.
Using these strategies helps everyone stay safe, calm down more quickly, and recover afterward.
Remember: Reducing the frequency and intensity of meltdowns involves using a combination of proactive strategies to prevent meltdowns before they happen, practicing regulation skills together with your child when they’re calm, and consistently applying de-escalation strategies when they’re needed.
Over time, this combined approach can lead to fewer and less intense meltdowns, benefiting both you and your child.
De-Escalation Strategies
Even with proactive strategies in place, meltdowns still happen. The following de-escalation strategies can help you safely navigate meltdowns by supporting your child effectively through their intense emotions.
Some of these techniques might initially feel like they’re telling you what NOT to do—That was intentional because a lot of our instinctive responses can unintentionally escalate the situation despite our best intentions. So I’ve tried to include the “what not to do” and the “what to do instead” to give the full picture.
1. Do Not Try to Use Reason or Logic – Focus on Safety and Reassurance
When your child is having a meltdown, the prefrontal cortex isn’t functioning the way it normally does. The stress response has flooded their body with adrenaline and cortisol, and they can’t access the part of their brain that processes logic the way they can when they’re calm.
It may be tempting to try to explain things or reason with your child. But mid-meltdown, reasoning attempts are almost always ineffective and can actually make your child more upset, because you’re asking their brain to do something it’s not currently capable of doing.
Avoid saying things like, “I know you wanted me to pick you up from school, but I have to work late.” or “Your pink shirt is in the washer, so I can’t have it ready in time; that’s why you need to wear a different shirt.”
An important distinction here: I’m not saying don’t show empathy. Simple validation (which we’ll get to in Strategy 4) can be helpful. But reasoning with empathy – trying to logically explain or solve the problem while also being kind about it – usually backfires at this stage. The logic part is the issue, not the empathy part.
Instead, focus on: Reassuring your child that they are safe, keep your language simple and minimal. Stay physically present and calm and meet basic needs.
Once your child has actually calmed down, they will be able to respond to reasoning. But mid-meltdown, it won’t help.
2. Avoid Making Demands – Put Expectations on Hold
Sometimes, too many demands can actually cause a meltdown in the first place, especially for children with a PDA profile.
PDA stands for Pathological Demand Avoidance. although many in the neurodiversity community have reframed this as “persistent drive for autonomy,” which better reflects the experience from the child’s perspective.
Rather than being oppositional, children with a PDA profile experience an anxiety-driven need for autonomy and can become deeply distressed when they feel controlled or pressured.
Regardless of the cause of the meltdown, avoid making more demands during it. Telling your child repeatedly to “stop,” “calm down,” or “snap out of it” isn’t going to make them stop or calm down. It doesn’t matter how nicely or assertively you ask.
Instead, focus on: Placing all of your other expectations on hold temporarily. The only thing that matters in the present moment is helping your child get through this. Everything else can wait.
3. Don’t Yell To Be Heard Over A Screaming Child – Use Calm Communication
If your child is having a meltdown, it’s best to maintain a calm voice.
Yelling makes you appear threatening (even if it’s not your intention) and will not help de-escalate a meltdown.
Once the stress response is activated, your child’s nervous system is perceiving threat. They need reassurance that they are safe.
You may think, “My child knows I’d never hurt them.”
Of course, logically, they do.
But during these situations, your child isn’t thinking logically at all. Their nervous system is reacting instinctually, so anything that seems threatening will worsen the situation.
Instead, focus on: Waiting until they stop screaming, and then speak calmly and empathetically. If you need to communicate something urgent for safety, get close, get low, and use a calm, quiet voice.
4. Validate Their Feelings, Not Harmful Actions
Everybody has the right to feel a certain way about any given situation. One thing you never want to do is shame your child for how they’re feeling.
Giving validation to their feelings shows your child that you accept their thoughts, feelings, and sensations.
This shows your child that you’re on their side. Even if you don’t think they have a “reason” to be upset, they obviously are, so try to put yourself in their shoes.
Say things like, “It makes sense that you are mad right now,” Or, “If that happened to me, I would be so upset, too.”
Include a “because” when you validate instead of a “but” – this is part of a strategy known as emotion coaching. You can read more on that here.
![18 Effective De-Escalation Strategies For Defusing Meltdowns 4 "Infographic titled 'Emotion Coaching' from Think Sensory. The graphic presents four numbered steps in arrow-shaped banners, alternating between teal and green, each paired with an example phrase on the right.
Step 1, Attend to the Emotion: Acknowledge something's wrong. Example phrase: 'Whoa! I can tell something's up right now.' Step 2, Name the Emotion: Use broad emotional language to reflect on what your child is experiencing. Example phrase: 'You seem really upset' or 'I can tell this feels really hard for you.' Step 3, Validate the Emotion: Remember, all emotions are valid, even if the behavior that accompanies them is challenging. Example phrase: 'It makes sense that you feel [emotion] because [reason 1], and [reason 2], and [reason 3].' Step 4, Meet the Need of the Emotion: Help your child get through the emotion until it passes. Example guidance: Sadness needs comfort. Fear needs safety and security. Anger needs patience, boundaries, and safety.
Below the four steps, the infographic reads: Emotion Coaching helps kids learn that feelings are normal, and they need to be experienced, not suppressed or avoided. It also helps them develop tolerance to sitting with uncomfortable emotions. The Think Sensory logo appears at the bottom."](https://thinksensory.com//wp-content/uploads/2026/02/Emotion-Coaching-2.png)
For example: “It makes sense that you’re upset right now because you really wanted the orange cup, not the blue cup – and because it’s hard not to get what you want sometimes.”
The difference between this and Strategy 1: Validation is simple and brief. It acknowledges what your child is feeling without trying to explain, fix, or reason through the situation. Reasoning with empathy (Strategy 1) is when you try to logically walk them through why something is the way it is, even kindly. During a meltdown, validation can help. Reasoning usually can’t.
You don’t want your child to feel shame for having emotions. We can learn a lot from emotions. When everyone is calm, you can always talk it out and guidance for next time.
A note on naming/Labeling emotions
During a meltdown, using simple, broad emotional language like “upset” or “mad” for the purpose of validation is a helpful tool. You’re not trying to teach your child how to identify, express, or label emotions in that moment. You’re trying to help them feel seen enough to start calming down.
But outside of crisis moments, it’s worth being careful about consistently labeling your child’s emotions for them. Research on interoception, particularly the work of Kelly Mahler, shows that when adults routinely tell kids what they’re feeling rather than helping them figure it out for themselves, it can actually undermine the child’s ability to recognize and trust their own internal signals over time.
Building that deeper emotional awareness is important work, but like all skill development, it happens during calm moments – through curiosity, open-ended questions, and letting your child lead. (You can learn more about interoception and supporting your child’s body awareness here.)
5. Respect Personal Space
Everyone’s personal “bubble” is different, but regardless, that bubble tends to get bigger with heightened emotions.
Unless your child asks, reaches for you, or communicates in their own way that they want you close, keep back at least 3 feet from them. Do not try to touch them, hug them, or pick them up (unless they’re in immediate danger and you need to intervene to keep them or others safe).
In a heightened emotional state like a meltdown, feeling trapped or closed in by you can further escalate the situation. This is especially true for children with sensory sensitivities, where unwanted touch during overload can feel genuinely painful or overwhelming.
6. Be Aware of Your Body Language and Facial Expressions
One of the biggest factors in de-escalation is caregiver emotional regulation. And a huge part of that is what your body is communicating, even when you’re not saying anything.
It’s important to appear calm and non-threatening throughout your child’s meltdown.
Check your facial expression: Consciously make sure you aren’t frowning, furrowing your brow, or clenching your jaw. Try to keep your expression neutral and soft.
Be intentional with your body language: Don’t cross your arms or put your hands on your hips. Avoid pacing, pointing your finger, or other large hand gestures. It’s best to keep your hands in front of your body in a relaxed position.
Remember, your child’s nervous system is scanning for threat right now. Even subtle cues from your body language can either help them feel safe or signal more danger.
7. Get Down to Your Child’s Level
Don’t stand over them, looking down at them as you talk. Standing above a child who is already in a heightened state can feel intimidating and threatening to their nervous system.
If your child will sit, sit with them. If not, kneel so you’re at eye level with them when communicating. (Although it’s usually best to keep communication to a minimum).
You may even need to lay with them if they’re on the floor if that’s what they’re doing.
8. Distraction (Circumstantial – Use Early)
This strategy is very situational, and it works best the earlier you use it. The closer to the initial trigger you can redirect, the more likely it is to help.
Once your child has moved into acceleration or beyond, distraction becomes much less effective because the nervous system is already too activated to be redirected by something external.
It’s also important to think about what’s driving the escalation, because distraction doesn’t work the same way for every type of trigger.
If your child is escalating because of an unmet physical need – they’re hungry, they need the bathroom, they’re in pain – distraction might buy you a few minutes (like if you’re stuck in traffic and your kid needs a bathroom), but it’s not going to resolve the situation. Meeting the need is what will actually help them feel better.
If the environment itself is the trigger – it’s too loud, too bright, too crowded, too unpredictable – distraction also isn’t the right tool. You need to adjust or remove them from the environment. No amount of redirection will help if the thing causing the overload is still happening around them.
Where distraction tends to work best is in situational frustration – moments where your child is upset about something that happened, they’re stuck on a problem, or they need a break from what they’re doing
In those moments, try offering a comfort item, a preferred calming activity, trying to make them laugh, or suggesting a short walk or offering your child a break in a calm-down corner. A change of scenery can help because it shifts the environment and gives the nervous system a chance to reset.
Once they’re calm and more capable of thinking clearly, you can re-address the original issue if appropriate.
9. Reflect on Your Child’s Wants and Needs
Reflective listening shows you are listening to their concerns, however poorly they are being communicated.
Say things like, “So you are saying you are upset because you really wanted your pink shirt today?” or ” You don’t want your Aunt to pick you up from school. Do I have this right?“
If you’re lucky enough to get a moment where your child says “YES!” to your reflection, it opens an opportunity for you to validate your child’s feelings then and help them calm down.
How this connects to Strategies 1 and 4: Reflective listening is different from reasoning. You’re not explaining or solving. You’re just repeating back what you’re hearing so your child feels understood.
It pairs well with validation (Strategy 4) because once you’ve reflected what they’re experiencing, you can follow up with “that makes sense because…” to validate it.

10. Acknowledge your Child’s Right for Refusal (Use Early)
A note about timing: This strategy works during the early stages of escalation. If your child is already in a full meltdown, they won’t be responsive to this approach. Save it for the moments when you can see things starting to build but haven’t peaked yet.
Children often become a lot more willing to cooperate when they don’t feel like they’re being forced to do something. This is especially true for children with PDA profiles. where perceived pressure or loss of autonomy can intensify distress and anxiety significantly.
Acknowledge this right by saying, “You’re right, I can’t make you do …” then explain why you would like them to choose to do what naturally follows from their choice.
The key word there is naturally.
The outcome you describe needs to be logically connected to the refusal, not an imposed punishment dressed up as a choice. If the two options you’re offering both feel bad to the child, or the consequence is unrelated to what you’re asking, it stops being a respectful acknowledgment of autonomy and starts being coercion with extra steps.
For example: “You’re right, I can’t make you put your shoes on. But, we can’t walk to the park until you have shoes on, because your feet need to be protected outside.”
The shoes and the park are logically connected – one literally can’t happen safely without the other. Compare that to something like, “Put your shoes on, or else you’re losing screen time tonight.” There’s no logical connection between shoes and screen time. That’s a punishment, and it undermines the whole point of this strategy, which is to give your child genuine autonomy within a boundary.
A few more examples of natural, logical connections:
- “We can’t start the craft project until the table is cleared off – we need the space.”
- “You don’t have to brush your teeth right now, but if it takes a long time, we might not have time for stories before bed because it’s time for lights out at 8.”
- “You don’t have to get in the car right now, but the movie starts at 2, so if we don’t leave soon, we’re going to miss the beginning.”
You’re allowed to set boundaries and allow them to choose. This approach gives your child a sense of control and autonomy, which may help reduce the anxiety driving their refusal. But it only works when the choices and outcomes are honest and logically connected.
If this is new to you, there’s a bit of a learning curve. It can take some practice to figure out how to identify and communicate the logical consequence of refusing something you want your child to do. That’s okay. It takes time.
A good starting point is to ask yourself why you’re making the request in the first place. The reason behind the ask usually points you straight to the natural consequence.
For example, if you’re asking your child to clear the table, why? Because you need the space to do the next activity. That’s your logical consequence right there – we can’t do the next thing until the space is available.
If you’re asking them to put on sunscreen, why? Because the sun will burn their skin without it. So the natural consequence is that they can’t go outside without sun protection.
When you get stuck, it’s usually because the honest answer to “why am I asking this?” is “because it’s the rule” or “because I said so.” That’s a signal to pause and think about whether there’s an actual logical outcome you can connect to, or whether this might be a situation where a different approach would work better or where you can actually let the demand go.
11. Answer Their Questions But Don’t Engage with Aggressive Statements
If your child asks a question during a meltdown, even if the tone is harsh or the way they’re asking feels demanding or aggressive, provide a calm and concise answer.
During a meltdown, your child doesn’t have access to their usual communication skills. A rough tone or forceful phrasing is what communication sounds like when the prefrontal cortex is running on fumes.
Answering their questions matters because it gives your child a small sense of being heard. Sometimes it can even crack open a tiny window toward de-escalation, especially if it leads to a moment where you can reflect back what they’re saying (Strategy 9) or validate what they’re feeling (Strategy 4).
Keep your responses short. Answer their questions and nothing more.
What you want to avoid is engaging with aggressive statements directed at you. If your child yells something like, “You’re the worst mommy in the world!” or “I hate you!” – don’t respond.
Don’t defend yourself, don’t correct the language, and don’t express hurt. Any of those reactions pulls you into a back-and-forth that usually escalate things further.
I know that’s easier said than done. Those words sting, even when you logically know your child doesn’t mean them. But what’s happening in that moment is that the stress response is doing the talking, not your child.
They don’t have access to the communication skills they’d normally use, so what comes out is big, raw, and aimed at whoever is closest. It’s not a reflection of how they actually feel about you.
Let it pass. You can talk about it later when everyone is calm.
And if aggressive communication is a pattern for your child when they’re angry, that IS worth addressing – just not during a meltdown.
This printable: Assertive vs Aggressive Communication can be a helpful tool to work through together during a calm moment to help them build those skills over time.

12. Silence
Sometimes, total silence can help your child begin calming down.
Stop talking altogether to both your child and anyone else around you. I also try to take slow, deep breaths when I’m trying this strategy. Breathe deeply enough that it’s audible in the silence.
This does two things. It helps you stay regulated (remember, co-regulation), and it models a healthy calming strategy for your child, even if they aren’t ready to use one themselves yet.
13. Offer a Movement Break or a Walk
Getting moving is a well-established way to reduce stress. Physical activity helps lower cortisol levels and supports the production of serotonin, and dopamine, which plays a role in mood regulation.
Ask your child if they want to go for a quick walk or movement break. You can even try this 7-minute HIIT workout for kids or these animal-theme gross motor skill activity cards if your child is open to it.
Movement can also serve as a natural transition out of the stress response by giving the body something active to do with all that built-up energy.
14. Be Non-Judgmental
This one is harder than it sounds, because judgment often shows up before we even realize it’s there.
When your child is melting down over something that seems small, or reacting in a way that, as an adult, feels disproportionate, it’s natural to feel frustrated. Especially if you’re also stressed, tired, or in public where people are judging you. That frustration can come out as judgment without you intending it.
Judgment can show up in a lot of different ways. For example:
- Sarcasm – “Oh, that’s real nice” or “Great, here we go again”
- Dismissing their feelings – “There’s nothing to cry about” or “You’re fine, it’s not a big deal”
- Blaming them – “Well, if you had just listened the first time, this wouldn’t be happening”
- Treating them as unintelligent – “I literally just explained this to you” or “How do you not understand?”
- Shaming – “You’re too old for this” or “Look at how everyone is staring at you right now”
These responses might feel small in the moment, but to a child whose nervous system is already overwhelmed, they land as shame. And shame doesn’t de-escalate anything. It makes your child feel worse about themselves on top of already feeling terrible, and it damages the trust between you that you need for co-regulation to work.
For neurodivergent kids in particular, judgment often comes from a gap between how adults expect them to respond and how their nervous system actually works. A 10-year-old melting down over a change in plans might look “too old for this” from the outside, but their nervous system doesn’t care about age-based expectations.
If the response is happening, it’s real, and it needs support regardless of whether it matches what we think is appropriate for their age or not.
When you notice judgment rising in yourself, that’s actually useful information. It’s a signal that your own stress is climbing and you might need to pause and check in with your own regulation before you respond. Take a breath. Remind yourself that your child isn’t giving you a hard time – they’re having a hard time.
15. Decrease Stimulation
When the nervous system is already overwhelmed, every additional piece of sensory input adds to the overload.
Even things that wouldn’t normally bother your child can become unbearable when they’re dysregulated.
Think broadly about what stimulation is in the environment.
- Overhead lighting
- Background noises – the TV, music, people talking, siblings or other adults watching,
- Strong smells
- Visual clutter
- Uncomfortable clothing, body temperature, seating, etc.
You know your child’s sensory profile best – start with whatever is most likely to be adding to their distress.
Minimize what you can. Dim lights, turn off screens, lower your own voice, and ask other people to leave the room if possible. The fewer inputs their nervous system has to process, the faster it can start to settle.
It’s also a good idea to have a safe, calming space where your child can go to remove themselves from the situation when they’re overstimulated.
Having this set up proactively (before a meltdown happens), with your child’s input on what feels good to them, so it’s ready and familiar when you need it.
16. Avoid Saying “No”
This strategy gets a lot of pushback, so let’s be clear about what this means and what it doesn’t mean.
This is NOT about never saying no to your child. Boundaries are important. You are absolutely allowed and expected to set limits.
This IS about strategically avoiding a known trigger word during a crisis. Those are two completely different things, and they get conflated a lot.
During a meltdown, when your child’s nervous system is already activated, and they’re in a heightened state, the word “no” is an additional trigger that makes things worse. The word “No” is a hard stop for the brain. When emotions are already elevated, it can feel like a wall going up. It intensifies the distress.
The common criticism here is that kids need to learn to accept “no,” and that avoiding it is somehow making kids soft or setting them up to fail in the real world. Teaching kids to accept no for an answer is a valid. Kids DO need to learn to handle hearing “no.” It’s an important skill. But you can’t teach a skill during a meltdown.
The part of the brain that learns, processes, and adapts isn’t available right now. So saying “no” mid-meltdown isn’t actually teaching your child to accept “no.” It’s just making the meltdown worse and longer.
You teach kids to tolerate “no” the same way you teach any other skill – during calm, regulated moments, with practice, over time. That’s when the learning happens.
And for what it’s worth, we extend this same logic to adults without thinking twice. If a coworker was having a panic attack, nobody would stand over them saying, “Well, your boss is going to tell you no sometimes, so you need to deal with it.” We understand that you help the person through the crisis first and deal with everything else after. Kids deserve that same consideration.
What to say instead of “No”
If your child asks you a question during a meltdown, instead of “no,” offer a more open-ended response. Something like, “We can plan a time to do that,” or “That’s something we can talk about when everybody is calm.”
You’re not saying yes. You’re not giving in. You’re just choosing language that doesn’t escalate the situation in a moment where everyone is already overwhelmed.
Once they’re calm, you can set whatever boundaries need to be set, including saying no.
17. Use Calming Visual Input
Certain types of visual input can be soothing and help children begin to settle.
Slow, repetitive, predictable visual patterns give the nervous system something low-demand to focus on, which can help shift it out of that high-alert state.
Things like calm-down bottles (glitter jars), lava lamps, LED light projectors, slow-moving sand art, or even watching fish in a tank can work well. Some kids also respond to visual stim videos – slow-motion clips, liquid pouring, sand cutting, things like that.
The key is familiarity. These tools work best when your child has already used them during calm moments, so their nervous system associates them with feeling safe and relaxed.
If the first time your child sees a calm-down bottle is mid-meltdown, it’s probably going to get thrown. Introduce them during positive, calm moments first.
18. Deep Breathing Exercises
The truth is, unless deep breathing skills are practiced with your child when they’re calm, they’re probably not going to work when they’re upset.
It takes a lot of practice and pre-teaching for a child to be able to use deep breathing exercises as a regulation tool. However, the work can pay off.
With frequent practice while calm, you’ll eventually be able to prompt your child to do deep breathing exercises when they’re upset, or you can model that breathing and have them imitate you. If you can get your child to use this strategy in the moment, it works quite quickly.
If not, deep breathing is also something you can do together during the recovery phase after the meltdown has passed.
Read some tips about how to teach kids to do deep breathing correctly: here
This 5-minute bio-feedback activity (done when everyone is calm) is a great way to show your child how deep breathing helps you calm down; it’s called How low can you go?
Finding What Works for Your Child
All of these strategies won’t work for all children, and the ones that do work probably won’t work every time.
But having a bank of de-escalation strategies to try is incredibly useful for parents who regularly navigate meltdowns.
As you try out these methods and learn how your child responds, you will find the best techniques for you.
You may also want to take some time to read: 8 Verbal De-Escalation Techniques for Managing Challenging Behavior & Meltdowns.
Free Printable De-Escalation Strategies Poster
Download these de-escalation strategies as an 8.5 x 11-inch poster below. You can use this poster to display as a visual reminder or to pass out as a handout.
De-Escalation Strategies Poster
Printable 8.5 x 11-inch poster of de-escalation strategies.
Use it as a poster, handout, or visual reminder.